Why your Weight and BMI are not the Whole Story
If you have ever stepped on a scale and felt confused — or even discouraged — by what you saw, you are not alone. For decades, weight and BMI (Body Mass Index) have been the go-to tools for assessing whether someone is "healthy" or not. But these numbers tell us surprisingly little. What truly matters is body composition.

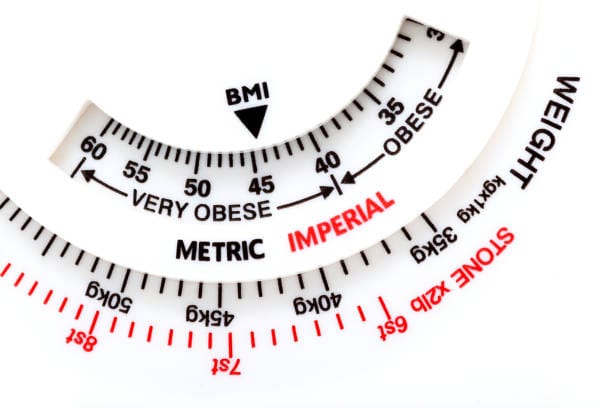
The standard BMI ratio (kg/m²) classifies adults as underweight under 18.5, as healthy between 18.5 and 24.9, overweight between 25 and 29.9, or obese above 30. While this is a useful population-level screening tool, it is not designed to assess individual health. It cannot distinguish between muscle, fat, water, and bone — and that distinction changes everything.
Two people can share the exact same BMI and look completely different, feel completely different, and have entirely different health risks. A professional athlete and a sedentary individual can both fall into the "overweight" BMI category, yet their metabolic health, cardiovascular risk, and energy levels may be worlds apart. This is why, in modern nutritional practice, body composition analysis has become an essential part of a thorough health assessment.
What is Body Composition ?
Body composition refers to the proportions of fat mass, lean mass (muscle, organs, bone), water, and other tissues that make up your total body weight. Body composition is typically measured using tools such as bioelectrical impedance analysis (BIA), DEXA scans, or skinfold callipers. These methods give us a far more nuanced picture than a simple scale ever could.
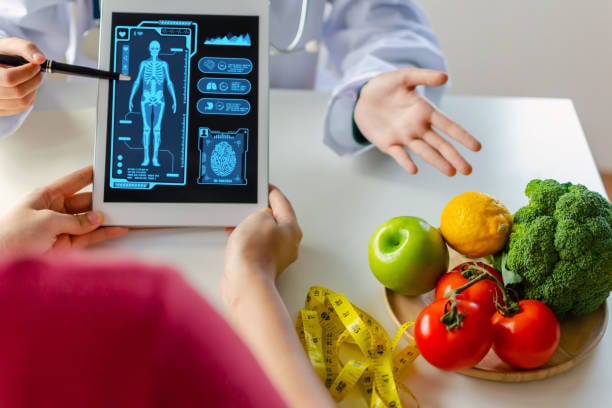
Subcutaneous Fat vs Visceral Fat : not all fats are equal
Fat is essential for your body and your general health. It is a key element for absorbing fat-soluble vitamins (A, D, E and K), producing hormones, protecting your organs, and keeping your brain and nervous system functioning. Without enough of it, these vital processes simply break down.
Healthy ranges for body fat percentage vary significantly by sex, age, and individual factors, but general guidelines suggest:
- Women: 20–35% is generally considered healthy;
- Men: 10–22% is generally considered healthy;
- Athletes of both sexes often sit at the lower end or even below
When we talk about body fat, it is essential to distinguish between two very different types:
Subcutaneous Fat
Subcutaneous fat is the fat stored directly beneath the skin. It has a protective function. Excess subcutaneous fat can be aesthetically concerning for some. It may carry some health implications but only at very high levels. Metabolically, it is relatively inert — which means it is not the primary driver of cardiovascular disease or insulin resistance.

Visceral Fat
Visceral fat is far more concerning from a medical perspective. This fat is stored deep within your body, surrounding vital organs including the liver, pancreas, and intestines. Unlike subcutaneous fat, visceral fat is metabolically active: it releases inflammatory molecules (cytokines) and disrupts insulin signalling, contributing directly to type 2 diabetes, cardiovascular disease, non-alcoholic fatty liver disease, and certain cancers.
You cannot really see visceral fat from the outside. Someone who appears slim may carry dangerous levels of visceral fat. A visceral fat rating of 1–9 is considered healthy ; 10–14 is high ; and above 14 is very high.
Waist circumference is also used as a proxy: a waist above 88 cm (35 inches) for women and above 102 cm (40 inches) for men is associated with significantly elevated metabolic risk.
Reducing visceral fat — through nutrition, stress management, quality sleep, and appropriate physical activity — is one of the most powerful steps you can take to protect long-term health. You can read more about how nutrition and inflammation are deeply linked on this site.
Muscle Mass: the metabolic engine you cannot afford to ignore
Muscle is heavy. Far heavier than fat. Muscle is roughly 18% denser than fat. A person who gains muscle while losing fat may see little change — or even an increase — on the scale, yet their body will look leaner, their clothes will fit differently, and their metabolic health will have improved significantly.

Muscle mass is critical for several reasons:
- Resting metabolic rate: Muscle is a metabolically active tissue. The more muscle mass you carry, the more calories your body burns at rest. Skeletal muscle accounts for approximately 20–30% of your total resting energy expenditure.
- Glucose regulation: Muscle tissue is the primary site for glucose uptake following a meal. Good muscle mass helps keep blood sugar levels stable
- Functional strength and independence : From the age of 30 onwards, we naturally lose 3–8% of muscle mass per decade — a process called sarcopenia which accelerates after 60. Preserving muscle mass is essential for mobility, balance, and quality of life as we age.
- Bone density: Muscle and bone are closely linked. Resistance-based activity that builds muscle also strengthens bones.
Losing muscle mass is never a good outcome, even if it causes the number on the scale to drop. Crash diets, extreme caloric restriction, and very low-protein diets are particularly harmful in this regard. You can learn more about why fad approaches fail in our article on diets.
For healthy adults, skeletal muscle mass should ideally represent around 33–39% of total body weight in women and 40–44% in men, though these figures vary with age and activity level.
Hydration: the overlooked component
Water is the most abundant substance in the human body, typically accounting for 55–65% of total body weight in adults. Like muscle, water is heavy.
This has enormous implications for weight fluctuations. It is entirely normal to see variations of 1–2 kg from one day to the next, purely due to changes in hydration status, sodium intake, hormonal fluctuations, or carbohydrate intake (which causes the body to store glycogen along with water). These daily swings have nothing to do with fat gain or loss.

Water retention (oedema) can also cause significant, visible bloating and weight gain. It may be linked to hormonal imbalances, high sodium diets, sedentary behaviour, or underlying health conditions. Addressing water retention through diet — for example, by increasing potassium-rich foods, reducing ultra-processed foods, and staying well hydrated — can lead to a noticeable reduction in scale weight.
Volume vs Weight: Understanding what you are actually trying to change
This is one of the most frequent clinical conversations I have with patients, and it is worth spelling out clearly:
If your goal is to lose volume — to drop a dress size and look visibly leaner
Then what you need to lose is volume, ie subcutaneous fat. Fat is light but voluminous: 1 kg of fat takes up far more physical space than 1 kg of muscle or water. This is why reducing body fat percentage has such a dramatic effect on how clothes fit, even when the change in scale weight seems modest. Losing 3–4 kg of fat, for example, can equate to dropping one to two clothing sizes. Do not be disheartened if the scale does not move dramatically — the volume loss is real and meaningful. Losing subcutaneous fat will require looking at sugar intake, portion sizes, physical activity and chrono-nutrition.
If your goal is to feel lighter for health reasons and get more more ease of movement
Then the conversation shifts towards water and water retention. Addressing oedema through dietary changes, movement, hydration and lymphatic drainages, you can obtain significant results quite rapidly. However, this must be done correctly — diuretic approaches or extreme fluid restriction are counterproductive and potentially dangerous.
And always protect muscle mass
Whatever the goal, losing muscle is not the answer. It would slow down your metabolism, reduce your functional capacity, and increase your risk of rebound weight gain. A well-designed plan will always prioritise muscle preservation — and ideally, muscle gain — regardless of whether the overall direction is weight loss or body recomposition.
Individual Variation: there is no universal target
One of the most important principles in clinical nutrition is this: there is no one-size-fits-all answer. Any plan should be personalised and professionally supervised.

Whether you want to lose fat, gain muscle, reduce visceral fat, address water retention, or simply improve your overall metabolic health, a generic plan carries real risks:
- Nutritional deficiencies: Restricting food groups or calories without professional guidance frequently leads to deficiencies that may not be immediately obvious but which have serious long-term consequences
- Muscle loss: Poorly designed weight-loss plans may result in muscle loss alongside fat loss, which slows metabolism and makes long-term maintenance nearly impossible.
- Metabolic adaptation: Repeated cycles of restriction and rebound (yo-yo dieting) cause metabolic adaptation, progressively making it harder to manage body composition over time.
- Psychological impact: Unsupported, rigid dietary regimens are among the risk factors for disordered eating, particularly in younger patients.
- Sustainability: The most effective nutritional approach is one you can maintain for life and that includes the pleasure element — not one you follow for eight weeks and then abandon. A personalised plan, built around your food preferences, lifestyle, culture, and goals, is infinitely more sustainable than any generic programme. If the plan is difficult to maintain, the results will be as difficult to maintain too.
A nutritionist or dietitian can assess your full body composition (not just your weight), identify your specific patterns, design a plan tailored to your individual metabolism and objectives, and provide ongoing (technical and emotional) support to make long-term change possible AND lasting.

Key Takeaways
- Weight and BMI are blunt tools. Body composition is far more clinically meaningful.
- Subcutaneous fat is the fat you can see and pinch; visceral fat surrounds your organs and is the more dangerous of the two.
- Muscle is heavy and dense; fat is light but voluminous. Losing fat changes how you look; losing muscle slows your metabolism.
- If you want to drop clothing sizes, you need to reduce volume — not necessarily scale weight.
- If you feel heavy, water retention may be a significant factor — and it responds well to dietary and lifestyle changes.
- Optimal body composition targets are individual: they depend on your genetics, age, activity level, metabolism, and health history.
- The foundations of healthy body composition are balanced, diverse meals, stable blood glucose levels and regular physical activity.
- Any plan to change your body composition should be personalised and monitored by a nutrition professional to be effective, safe, and sustainable long-term.
Francine Joyce is a registered nutritionist practising in London, specialising in personalised nutrition for metabolic health, weight management, and eating disorders. To book a consultation, please visit the contact page.



